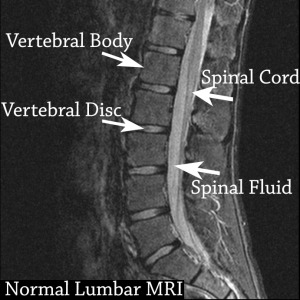
What is a vertebral disc?
A vertebral disc is the shock absorbing cushion between vertebral bodies. They exist at every level between C2 and S1. They are held in place by annular fibers, a criss-crossing dense fiber mesh that anchors into the bone of the vertebral segment. These fibers flex and bend, allowing the disc to expand slightly, as the spine moves forward, backward, and to both sides. This gives the entire spinal column a very effective spring like effect, to ensure that it is a load bearing structure. With normal function, the spinal column can withstand incredible compressive force that would otherwise be traumatic, to other joints. The center of the vertebral disc is a denser substance known as the nucleus pulposus. This denser region gives the disc a stable center, as well as a pivoting point, that prevents the center of the vertebral body from crushing the center of the disc.
What is a disc herniation?
A disc herniation goes by many names. It seems many people (including some medical professionals) have their own names for them (slipped disc) but they all mean the same thing. Colloquialisms aside (discs can’t actually “slip”) a disc herniation is when fibers (known as annular fibers) around a vertebral disc rupture. The motion that causes this rupturing is almost always a motion that puts incredible strain on the dense center of the disc, known as the nucleus pulposus. This causes the nucleus pulposus to shift from its home in the center of the vertebral disc, away, toward the rupture. The surrounding disc material, which is less dense, is pushed outward through the ruptured fibers. If this happens on the anterior of the spinal column, you’re in luck. There isn’t as much important stuff out there. Dense ligaments on the anterior side of the spinal column typically retain the herniation, and the overall segment loses some height. This may still cause pain, and early degeneration, but it is not nearly as bad as a posterior herniation can be. If the herniation is posterior, the disc material still has a dense ligament sheath that will normally retain its contents, but the bit of disc that does push outward, pushes into the spinal canal.
Are disc herniations dangerous?
Herniations can cause a litany of problems, depending on the where the herniation occured. Anywhere below L2, you don’t have a “spinal cord” per-say, just a bundle of thick nerve roots. At this level and below, the spinal column more closely resembles hanging cooked spaghetti, which travels down, through the rest of the spine, exiting through the vertebrae and inserting into the muscles of the feet and legs. These nerves are much more forgiving to be intruded upon, than the spinal column itself. Lumbar herniations are typically more forgiving than cervical herniations, but are much more common than cervical injuries. However, both can be completely debilitating. There is no intending to down play either injury. The higher up the spinal column the injury is, though, the worse the symptoms can potentially be. The nerves to the feet must travel from the brain, just the same as the nerves to the arms. Given that the nerves from the feet are traveling through the spine to the brain, a significant spinal injury to the neck can possibly cause problems in the legs, where a spinal injury in the lumbar area, cannot cause neck pain.
Problems from disc herniations can be numerous, because the spinal cord is sending all bodily function information from the brain, or to the brain. It entirely depends on where the herniation is, and what kind of damage is done to the cord. Anterior disc herniations don’t impinge on the cord, as previously mentioned, but the vertebral levels that they may occur at, still correlate to specific nerves traveling to and from the vertebral column, to the body. Just because there is no direct cord compression, doesn’t mean the nerves in that area can be inflamed or damaged as a result of the reduction in vertebral disc height. Generally speaking, disc herniations can cause, numbness, tingling, burning, shock like sensations that span large, defined areas, from the spine outward. If there is significant compression or inflammation, near specific spinal nerves, muscles that they innervate may atrophy (lose muscle mass), coordination of specific joints can become diminished, or it is also possible that there is no effect from the injury at all. It all varies as per how your body responds to the injury.
It’s possible to have a herniation and not know it?
Absolutely! A study1 was conducted on 67 participants. Every participant received an MRI looking for lumbar abnormalities. The results found that 20% of the patients under the age of 60, had disc herniations, while 57% of the patients over the age of 60 had disc herniations. All of these disc problems were completely without pain, or symptoms. Once the disc ruptures through the annular fibers, there is no guarantee that it is going to get worse. The body might inflame the area, repair the damage as best possible, and heal with very dense scar tissue, holding the herniation in place. After the inflammation subsides, the local tissues no longer report back the brain that the area is injured, so even though the herniation remains, there is no pain provocation from the event. There are also others who exhibit herniation like symptoms, with very minor herniations present. The body is very complex, and if tissues become inflamed, you will experience pain. If you have a lot of building blocks in your body for inflammatory processes to develop and be produced, minor injuries will feel much worse than they should. This is why a healthy diet is key to healthy living.
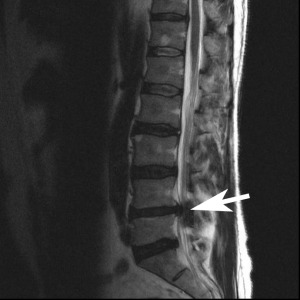
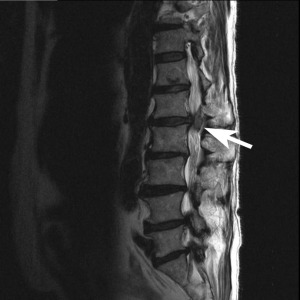
Below are two images, which one looks more painful?
These two images are both “bad” for the patient, but you cannot tell the extensive injuries by simply looking at an image. There is no pain visible in either of them. Letter A is a significant herniation, pressing directly on the spinal canal, and impeding on the spinal cord itself. Letter B, has a piece of vertebral disc that has broken off within the spinal canal (known as a sequestration) and has migrated upwards.
As partially stated in the last section, disc herniations do not necessarily hurt. For example, if an MRI was conducted, and you could see a disc herniation (annular tear/disc rupture/disc extrusion/etc) with surrounding inflammation, there is a great clinical indication that, that location is a source of pain. However, this advanced testing cannot detect pain. It is simply a test that needs to be added to the impression already determined by the physician. Some patient’s have herniations visible on MRI with no pain, and no reproducible pain with testing. Is it still a herniation? Yes. Is it clinically significant, not really. However, this is not to undermine the possible pain experienced by an active disc herniation. They can be debilitatingly painful. Some patients have regarded disc herniation pain worse than child birth. These statements vary, of course, due to the complexity of each injury, and the particular person experiencing it. The simplest way to state this is that disc herniations can vary from non-painful to excruciating. The best way to reduce the amount of pain felt, is to have the area properly treated by a skilled practitioner, to exercise as best possible (as directed by the practitioner or trainer), and to maintain a healthy, well rounded diet. Not only will this minimize the amount of inflammation, naturally, but it will also allow the area to heal, as well as maintain proper joint motions.
With reference to images A and B above. Image A has cauda equina syndrome, known as complete loss of function of the muscles and structures of the “saddle” area of the pelvis. While Image B is paraplegic from the legs down, without any “saddle” disruption. Both of these cases are no longer considered “conservative” with terms of treating, they are immediate surgical candidates. Disc injuries range from non-painful, to extremely painful, to absolute medical emergencies.
How are disc herniations treated?
Conservative treatment is generally accepted as the first path of care when it comes to treating a disc herniation. This, of course, requires the injury to be properly assessed. If there is gross loss of function, then the injury is typically immediately determined to be surgical. Short term loss of function from a spinal injury may heal in time, as long as the spine itself isn’t damaged. Long term loss of function greatly reduces the chances of that injury healing properly and completely.
Conservative treatment consists of chiropractic treatment, physical therapy and possibly personal training. The idea of these treatments are to reduce (called centralizing) the herniation, give time to allow the injury to heal, and then strengthen the area to prevent a recurrent injury. The main cause of disc herniations is improper force loading of the spine. Re-educating the body on how to properly move as well as strengthening the muscles to be more resistant to the amount of force the person is required to use, will better prevent the injury from occurring in the future.
Conservative care is regarded as the first measure for care, because many patients experience good results and fast recovery with proper treatment. If the pain does not improve, or the symptoms reduce, then the patient has been properly screened for a surgeon. The manual therapist should have well documented the case, the level of injury, and what type of treatment failed. This information, when passed along to the surgeon gives him/her an excellent idea of what exactly needs to be operated on, thus dramatically increasing the success rate of the operation. The last note for why conservative treatment is generally regarded as a “first method” is because it has an excellent track record (with skilled practitioners) and if surgery is conducted first, and isn’t successful, it cannot be undone. Conservative treatment is very unlikely to further damage the patient. If surgery is done first, and the anatomic area is dramatically changed during the operation, this can directly cause later conservative treatment to dramatically decrease its effectiveness, or greatly increase the length of treatment.
Here at Herrington Family Chiropractic, LLC, I have studied extensively to thoroughly understand the spine, its movements, and injuries. I’ve specialized in treatments pertaining to such conditions as explained above. Proper treatment is important, but proper assessment is even more so. I pride myself on being able to isolate the source of your pain, and if necessary, making the proper and prompt referral to an orthopedic surgeon get you the best care if needed.
Click the Contact Us link at the top to call and schedule an appointment!
1 Boden, S., Davis, D., Dina, T., Patronas, N., & Wiesel, S. (n.d.). Abnormal Magnetic-Resonance Scans of the Lumbar Spine in Asymptomatic Subjects. A Prospective Investigation. Journal of Bone and Joint Surgery, 72(3), 403-408. Retrieved from http://jbjs.org/content/jbjsam/72/3/403.full.pdf